Sleep apnea is very common in patients with heart problems. In fact, it affects up half of patients with heart failure and/or atrial fibrillation.1,2 Sleep apnea may worsen some of the symptoms that cardiologists hear about the most from patients—trouble sleeping, fatigue, daytime sleepiness, and decreased ability to focus.3,4 As a result of increasing evidence linking sleep and heart health, cardiologists are talking to more of their patients about sleep apnea.

“Central” sleep apnea – a form of sleep apnea that’s common for cardiology patients
When most people think of sleep apnea, they are actually thinking of Obstructive Sleep Apnea (OSA). OSA is the most common form of sleep apnea in the general population. In OSA, the breathing muscles (e.g. diaphragm) are activated appropriately but a narrowing of the passages in the upper airway (the tongue or throat) cause a blockage that prevents air from flowing freely. The obstruction can be due to bodily features or a relaxation of the muscles in the chest and neck during sleep.5
The story is more complicated for cardiology patients, especially those with heart failure and atrial fibrillation. In these patients, another form of sleep apnea—Central Sleep Apnea (CSA)—is nearly as common. In CSA, the brain fails to send regular signals to the breathing muscles. The lack of consistent signals leads to irregular nighttime breathing and poor sleep quality.5
The only way to determine which type of sleep apnea you have is to get a sleep study. Unfortunately, many cardiology patients find they have both types.
What’s causing my fatigue and poor sleep? Is it my heart, sleep apnea, or both?
Symptoms of sleep apnea, and especially central sleep apnea, can be difficult to spot in patients with heart failure and atrial fibrillation. Symptoms vary between patients and not all patients recognize their symptoms. Obvious symptoms such as snoring are not usually associated with central apneas.
Some symptoms overlap with symptoms of heart problems. People may incorrectly assume it is their heart that is causing fatigue and sleepiness, when in reality sleep apnea is a major cause. The only way to determine whether you have sleep apnea is to take an overnight sleep study. These can be done in sleep centers overnight or in your home with specialized equipment.
How does central sleep apnea impact the heart?
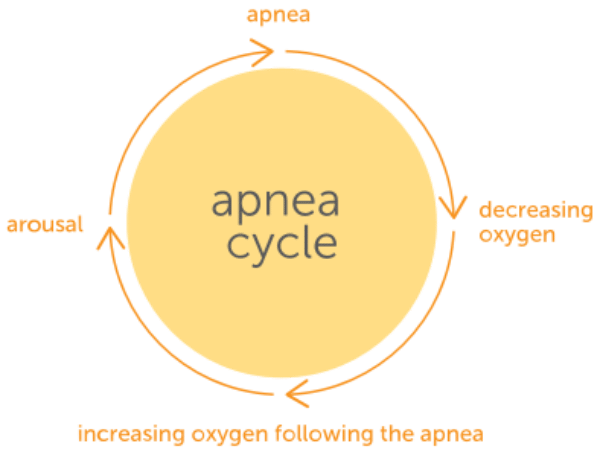
Central Sleep Apnea may have a negative impact on heart health due to apnea cycle. People with central sleep apnea, especially those with heart failure, tend to go through repeated cycles of:
- apnea
- decreasing oxygen
- increasing oxygen following the apnea
- arousal
This may cause:3
- Repeated activation of the “fight or flight response” (sympathetic nervous system): This increases heart rate and blood pressure, increasing the overall demand on the heart
- Heart stress from changing oxygen levels:
Repeatedly changing levels of oxygen in the blood can cause stress on the heart
- Inflammation: Increased inflammation can reduce the heart’s ability to pump blood effectively
- Constriction and clotting of the blood vessels:
Restriction in blood flow forces the heart to work harder
Repeating the apnea cycle throughout the night may partially explain the increased risk for patients with central sleep apnea and heart failure.3
Short and long-term consequences of untreated central sleep apnea for cardiology patients
Central Sleep Apnea can have a variety of symptoms presenting during the night and during the day.3,6
| Common nighttime symptoms | Common daytime symptoms |
|---|---|
| Trouble going to sleep and/or staying asleep | Daytime sleepiness |
| Episodes of shallow or paused breathing | Fatigue |
| Shortness of breath | Memory and concentration problems |
| Frequent (2 or more) trips to the bathroom | Headaches |
Beyond the short-term symptoms, sleep apnea has even been shown to increase the risk of hospitalizations and death for patients with heart failure. This may be due to the increased stress that apnea events put on your heart.7,8
Treatment options for patients with central sleep apnea
Physicians recommend various treatment options for people with central sleep apnea. Three of the options are detailed below.
Implantable Phrenic Nerve Stimulation (the remedē system)
remedē® is an implantable pacemaker-like device that activates automatically each night to stimulate your breathing muscles as you sleep. remedē sends signals via the phrenic nerve that cause your breathing muscles to contract, drawing air into your lungs, just as in normal breathing. The result is a more normal breathing rhythm and pattern.9
CPAP Machine
Continuous Positive Airway Pressure (CPAP) is a mask-based therapy that delivers pressurized air that opens a patient’s airway. Although it is designed for patients with obstructive sleep apnea, some patients with central sleep apnea see improvement in the severity of sleep apnea and symptoms.8
ASV Machine
Adaptive Servo Ventilation (ASV) is a type of positive airway pressure device. Similar to a CPAP, it uses a mask to deliver pressurized air that opens the airway and/or “deliver a breath.” The amount of pressure varies to smooth out the breathing pattern. ASV can improve the number of apnea and hypopnea events in some patients. Importantly, ASV should not be used for patients with heart failure and reduced ejection fraction, as studies showed increased risk of death for these patients.10
Closing
Sleep apnea, and especially central sleep apnea, is common for patients with heart problems. Sleep apnea may be contributing to your daily symptoms and increase your long term health risks. Consider talking to your doctor to learn more.




